ICF model and two functional impairments and two activity limitations
Patient details is below:
Diagnosis: Left middle cerebral artery cerebral vascular accident eight years post onset.
History: The patient underwent an angioplasty and following surgery suffered a heart attack and a stroke. She was comatose for 21 days.
Social: The patient is married. She enjoys gardening and sewing. She states she would like to work and has tried working at McDonald’s but this was too fatiguing for the hours that they wanted her to work. Prior to her CVA, she was a truck driver. There are no steps to her home. She has a scooter and uses it in the community, as she likes the freedom it gives her. She does drive a car.
Additional Assessment Information:
Right upper extremity: The patient reports she uses right arm and hand minimally in sewing and gardening, States she primarily uses her left upper extremity for activities of daily living. She was right hand dominant prior to CVA.
Transfers: Independent in bed, toilet, and car transfers. She reports she does get assist from her spouse to transfer on a tub bench for showering.
Ambulation: Ambulates independently in the home without assistive device. Short community distances are also independent without assistive device. States she uses a scooter for longer community distances. Reports she has never used an ankle foot orthotic (AFO). She reports she needs a railing or outside support on curbs, and stairs. Patient states she fell while gardening under low light and currently has bruises from this fall. She also reports falling is not a problem. Spouse adds that falling is not a problem unless she trips over her right foot.
Assignment Questions:
1. Considering the ICF model, list two functional impairments and two activity limitations that V.H. experiences.
2. List one objective balance measure that you would use to measure fall risk in this patient. Why you choose that test?
3. What test would you use to help determine this person’s ability to be a community ambulator? Why?
4. What standardized test could you use to measure participation (as defined in the ICF Model) or quality of life? Why would you select this test?
5. Since it has been 8 years since V.H. had a CVA, speculate what types of secondary (indirect) functional impairments and activity limitations she might have acquired.
This study describes some important concepts of International Classification of Functioning, Disability and Health (ICF) model of Functioning and Disability of a person. This study relates with the case study of a person who is facing serious issue of Left middle cerebral artery vascular. She cannot use her left side for dealing with different conditions of her health. This study delivers aspect of objective balance measure for measuring the fall risk of the patient. This study also describes the necessary impairment of function of physically disabled person.
Morse Fall Risk Assessment as one objective balance measure
ICF model refers to the International Classification of Functioning, Disability and Health (ICF) model of Functioning and Disability of a person. This ICF model helps to describe the as well as organize the information on disability or functioning of a person. It gives the scientific basis of understanding the health condition of a person. An ICF model includes within different components or domains.

Figure: ICF model
(Source: Ptjournal.apta.org, 2016)
For the particular context of this case study, ‘body function’ and ‘activity’ are much related components of the ICF model. ‘Body function’ is involved within the disability of mental function, pain and sensory function, speech and voice function, immunological as well as cardiovascular function and function of skin related structures (Hoang-Kim et al., 2014).
The ‘Activity’ is related to the aspect of learning and applying the knowledge into daily experience of a person. Activities are also related to proper way of communication, mobility or self care and domestic care of one person. ‘Activity or Participation’ is also included within interpersonal relationship or interaction. A person should also be involved within different gatherings of social, civic and community (Horak & Mancini, 2013).
The concerned person is diagnosed with Left middle cerebral artery vascular issue. According to the ICF model, her physical activities and body function have changed for her serious accident. She cannot use her left hand and left side as well due to the constraints in body. She only takes the help of her spouse to transfer on the tub bench for showering. Her left part is very weak as she performs different works with her right part of body.
For this context, Morse Fall Risk Assessment has been used by the author. Morse Fall Scale or MFS is considered as a simple and rapid method for assessing the likelihood of falling of a patient.
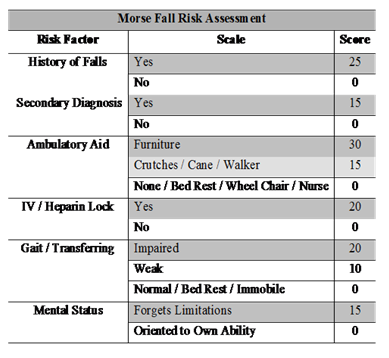
Figure: Sample of Morse Fall Risk assessment scale
(Source: Shumway-Cook & Woollacott, 2007)
Janie Morse has recommended this scale for assessing the level of risk of every person. 45 and more than 45 is included in the category of ‘High Risk’. 25-44 Score is involved in Moderate risk of the person. On the other hand, the score 0-24 is involved in the category of Low Risk of the concerned person (Hoang-Kim et al., 2014).
It is very much research driven. The process of interventions is standardized by the level of risk of every person. Most of the nurses and medical personalities use this scale as they consider this scale very easy to use. Different medical personalities have used MFS widely for the use of acute care setting. This risk assessment measure can be used both in long term setting of care as well as hospital setting (networkofcare.org, 2016).
Ability to be a community ambulatory
Ambulation for the people, who had undergone a stroke, can be evaluated considering a few measures like activity, impairment, participation and quality of life related to health. We can consider the Berg Balance Scale for this purpose. BBS includes some activities for the assessment of functional mobility. The activities are sit to stand, sit and stand without any support, stand with closed eyes, transfers, retrieve objects from floor, turn to look behind, stepping on a stool, standing for a while on one foot, standing on the feet in front of each other, turn 360 degrees etc (Ptjournal.apta.org, 2016).
These factors can determine a stroke patient’s ability to be a community ambulator. After a cerebral vascular accident and stroke, the nervous system along with blood circulation gets affected, which causes an adverse effect on reflex based activities and muscle function. By doing this assessment, an expert can understand the condition of her muscle functions and reflex. According to that, it can be decided that up to what extent she can be able to ambulate (Hoang-Kim et al., 2014). It has evidenced that there are evidences where individual with stroke experienced various rehabilitation all the way through acute and sub acute phases. Still, the walking habits largely influenced subsequent to stroke.
The World Health Organization Quality Of Life instruments or WHOQOL instruments can be the suitable method of determining the quality of life. It considers several factors like patient’s physical health, psychological conditions, a level of independence, environment, social relationship, environment and spirituality or personal belief (Mitra, 2014).
All these factors are related to a person’s mental and physical health. In this case, the physical health of the individual should be a primary consideration. After the cerebral vascular accident, many environmental issues like fatigue, muscle functions disorders, etc. are the major questions that affect or restricts the participation or quality of life. In this context, it has noted that there is 8 +1 dimensions of quality of life exist that required to be taken care of. These are material living conditions, productive or main activities, overall experiences of life, natural and living environment, education, leisure and social interactions, economic and physical safety, and government and basic rights (Hoang-Kim et al., 2014). The environmental conditions should also be taken into consideration as the patient has certain restrictions of working, daily living and travelling. Mental health is also important because a stroke patient should not feel the mental stress and needs a peace of mind (Shumway-Cook & Woollacott, 2007).
Stroke is affected by the interruption of blood supply in brain which may cause dysfunction of heart and nervous system. Beside physical impairment it can also cause cognitive impairment. With age the impairments also increases and may lead to hypertension, diabetes, artial fibrillation etc. The patient can have paralysis, weakness and problems with balance and coordination. A sensation of pain, numbness or tingling or burning may develop. Patient may feel fatigue even after a very light work. In some cases one side of body may not have any sensation or may not function properly.
To export a reference to this article please select a referencing stye below:
My Assignment Help. (2016). The ICF Model Assesses Impairments Of A Stroke Patient In An Essay.. Retrieved from https://myassignmenthelp.com/free-samples/international-classification-of-functioning-disability-and-health.
"The ICF Model Assesses Impairments Of A Stroke Patient In An Essay.." My Assignment Help, 2016, https://myassignmenthelp.com/free-samples/international-classification-of-functioning-disability-and-health.
My Assignment Help (2016) The ICF Model Assesses Impairments Of A Stroke Patient In An Essay. [Online]. Available from: https://myassignmenthelp.com/free-samples/international-classification-of-functioning-disability-and-health
[Accessed 31 May 2025].
My Assignment Help. 'The ICF Model Assesses Impairments Of A Stroke Patient In An Essay.' (My Assignment Help, 2016) <https://myassignmenthelp.com/free-samples/international-classification-of-functioning-disability-and-health> accessed 31 May 2025.
My Assignment Help. The ICF Model Assesses Impairments Of A Stroke Patient In An Essay. [Internet]. My Assignment Help. 2016 [cited 31 May 2025]. Available from: https://myassignmenthelp.com/free-samples/international-classification-of-functioning-disability-and-health.
